Research Meta-analysis for Physiotherapy in Parkinson Disease 🧠💪🦵 is further described as follow:
Abstract Background:
Physiotherapy is a commonly prescribed intervention for people with Parkinson’s disease (PD).
Conventional types of physiotherapy have been studied extensively while novel modalities are being developed and evaluated.
Objective:
To evaluate the effectiveness of conventional and more recent physiotherapy interventions for people with PD.
The meta-analysis performed as part of the 2014 European Physiotherapy Guideline for PD was used as the starting point and updated with the latest evidence.
Methods:
We performed a systematic search in PubMed,CINAHL, Embase and Web of Science. Randomized controlled trials comparing any physiotherapy intervention with no intervention or sham treatment were included.
Trials were classified into 12 categories:
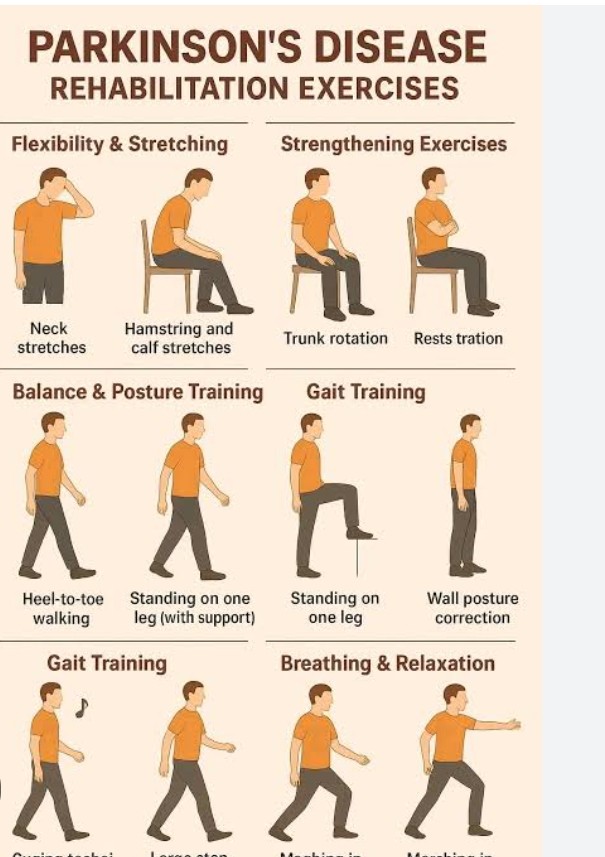
Conventional physiotherapy, resistance training,treadmill training,strategy training, dance,martial arts,aerobic exercises,hydrotherapy,balance and gait training,dual tasking,exergaming and Nordic walking.
Outcomes includes:
Motor symptoms,balance,gait, and quality of life and are presented as standardized mean differences.
The GRADE (Grading of Recommendations, Assessment, Development and Evaluation) approach was used to systematically appraise methodological quality.
Results:
A total of 191 trials with 7998 participants were included. Conventional physiotherapy significantly improved motor symptoms, gait and quality of life.Resistance training improved gait.
Treadmill training improved gait.Strategy training improved balance and gait.
Dance, Nordic walking, balance and gait training, and martial arts improved motor symptoms, balance and gait.
Exergaming improved balance and quality of life. Hydrotherapy improved balance.
Finally, dual task training did not significantly improve any of the outcomes studied.
Conclusions:
This meta-analysis provides a comprehensive overview of the evidence for the effectiveness of different physiotherapy interventions in the management of PD allowing clinicians and patients to make an evidence-based decision for specific treatment modalities.
Further work is needed to directly compare the relative efficacy of the various treatments.
Keywords:
European Physiotherapy Guideline; Parkinson’s disease; guideline; meta-analysis; physiotherapy; review.
Summary Of Article By PHYSIOHEALER:
A broad body of evidence suggests physiotherapy interventions provide at least small-to-moderate improvements in gait, balance, mobility, and daily functioning for people with Parkinson’s disease (PD).
Benefits are most consistently seen for targeted gait and balance programs and tend to be maintained with regular, ongoing practice.
– Interventions With Strongest or Most Consistent Evidence:
– Gait training with cues and/or treadmill-based programs: improves gait speed, stride length, and sometimes balance.
– Balance and postural control training: reduces fall risk and improves balance measures.
– Resistance/strength training: increases lower-limb strength and can improve functional mobility.
– Tai Chi and dance-based programs: improve balance, mobility, and sometimes QoL; benefits may accumulate with longer programs.
– Multimodal or supervised programs that combine elements (aerobic + resistance + balance) tend to yield robust improvements.
– Outcomes:
– Gait speed and stride parameters improve.
– Timed Up and Go (TUG) and other mobility measures improve.
– Balance scores improve; fall risk may decrease with regular training.
– Activities of daily living may improve, with QoL benefits reported in some studies.
– Practical considerations:
– Dose Matters:
Progression, frequency (often 2–3 sessions/week or more), and duration (several weeks to months) influence outcomes.
– Supervision plus home exercises tends to yield better results than home programs alone, though adherence is key.
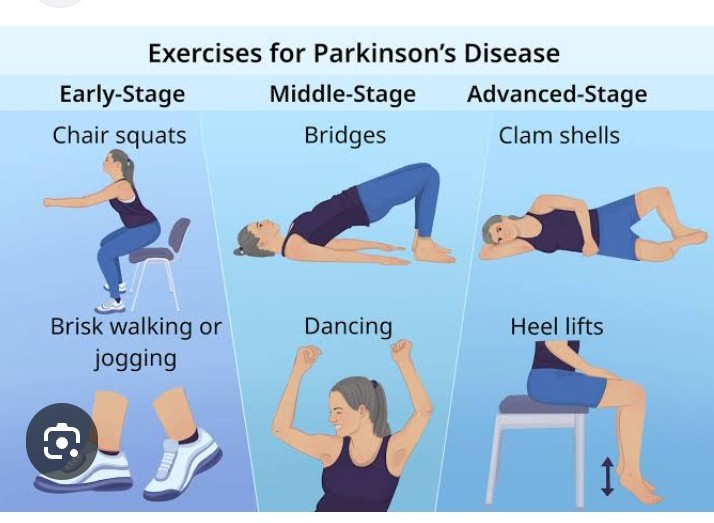
– Stage of PD and baseline impairment influence which modalities are most effective.
– Limitations And Gaps:
– Heterogeneity across studies in PD severity, outcome measures, and intervention protocols.
– Some evidence of small study effects and variable risk of bias.
– Long-term maintenance and optimal sequencing of modalities require more research.
– Practical Takeaway For Decision-Making:
– For Gait And Mobility Limitations:
Prioritize gait/locomotor training with cues,Consider treadmill-based options.
– For balance and fall prevention: incorporate balance-focused activities (e.g., Tai Chi, balance training) 2–3 times per week.
– For overall function and strength: add progressive resistance training.
– When possible, use a multimodal program, supervised initially, with a guided home program for maintenance.
